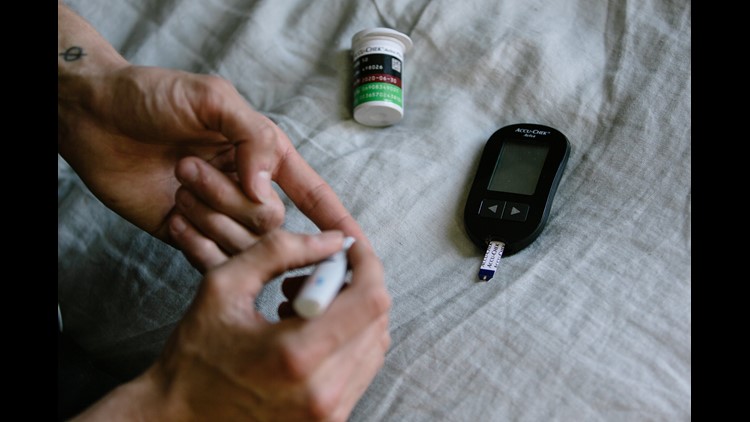
(CNN) — Tall people might be at greater risk of developing cancer, but short people aren’t off the hook.
Shorter people are at greater risk of developing type 2 diabetes, according to a study published Monday in the journal Diabetologia.
Researchers looked at more than 2,500 middle-aged men and women in Germany from a pool of about 26,000 people. After adjusting for age, lifestyle, education and waist circumference, researchers found that greater height was associated with a lower risk for diabetes.
The team evaluated height by taking into account both sitting height and leg length. The heights ranged from under 5’6″ (169.7 cm) to above 5’11” (180.3 cm) for men and under 5’2″ (157.8 cm) to above 5’6″ (168.1 cm) for women.
It found that, for both men and women, the risk of diabetes was lower by more than 30% for each three inch (10 cm) difference in height.
Part of the association between greater height and a lower risk for diabetes may come from the associations between greater height and lower liver fat content and other diabetic risk factors, like blood lipids, said Matthias Schulze, an author on the study, in an email.
The study also argues that shorter people should be monitored for diabetes and risk factors related to cardiovascular disease. Because liver fat contributes so much to the higher risk in shorter individuals, reducing liver fat may provide a way to reduce the risk of diabetes.
Gail Melkus, associate dean for research in NYU’s Rory Meyers College of Nursing and a diabetes researcher, called the study “a piece of the pie” in researching diabetes. Melkus is unaffiliated with the study.
“I think that the conclusions have to be cautiously interpreted because it’s a secondary data analysis, meaning they didn’t get a group of people and follow them going forward,” she told CNN.
She said the study poses an interesting question: Should short stature be another risk factor for screening for type 2 diabetes, along with family history or obesity? More research needs to be done to determine the answer.
Still, she said short people shouldn’t automatically think they’re destined for diabetes, nor should tall people think they’re safe and sound, especially other risk factors apply to them.
“It’s not just one risk factor that we need to consider when screening people for any health condition,” she said.
What is Type 2 diabetes?
Type 2 diabetes is pretty common. It affects about 1 in 10 Americans, according to the Centers for Disease Control.
Here’s how it works: Everybody produces insulin, a hormone made by our pancreas that allows blood sugar into our cells to use as energy. But when your body does this too much — pumping out insulin to get all that glucose into cells — the cells might stop responding and become insulin resistant. That leaves too much sugar in the blood, leading to high blood sugar and, you guessed it, type 2 diabetes.
Type 1 diabetes, on the other hand, is a completely different problem. People with type 1, an autoimmune disease, don’t make enough insulin and have to take it to survive.
The typical prevention methods for type 2 diabetes are increased physical activity — which helps make our bodies more sensitive to insulin — and weight loss. Avoiding high blood sugar and reducing stress help too, according to the CDC.